Temporomandibular Joint Disorders
General overview
Temporomandibular (or jaw joint) disorders are a common problem and occur in up to one third (1 in 3) of the population. The majority of people who have these disorders do not require management in hospital and cope with their symptoms such as clicking, occasional pain or mild restriction of opening. Of those who are referred for hospital consultation the majority can be managed very simply and do not require open joint surgery.
Most people with these disorders do not progress on to develop anything serious or worrying, such as arthritis.
Cause
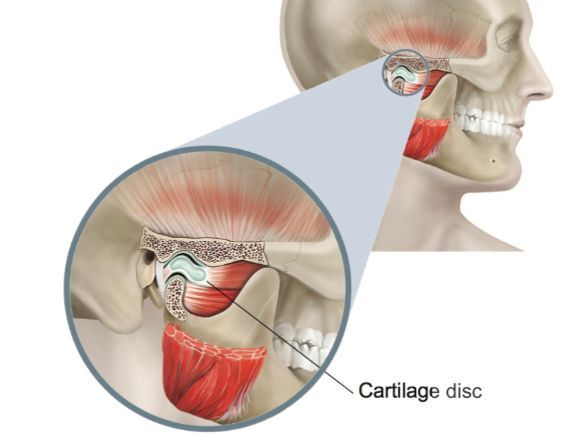
The “normal” jaw joint consists of the lower jaw, a cartilage disc in between and the base of the skull. The first couple of centimetres of opening occurs by rotation of the lower jaw against the cartilage disc and the subsequent mouth opening is by sliding of the lower jaw and disc along the base of the skull.
The jaw clicks in about one third of the population because the position of the disc is slightly anterior (forward) to that which is considered “normal” although this position can be considered to be a normal variant. In these cases, the first portion of opening occurs between the lower jaw and the tissues which lie behind the disc (the retro-discal tissues). These normally adapt to the extra force put upon them by movements of the jaw. The initial rotation occurs in the usual manner and then, on sliding the disc clicks back into its more “normal” relationship with the lower jaw to complete the opening path. This is what causes the click within your jaw joint.
Occasionally, due to injury or other problems, inflammation may develop within the retro-discal tissues and this causes pain around the joint, similar to that which you would sustain if you were to sprain a joint. When a joint is sprained you get pain in and around the joint but you also get pain in the muscles around the joint. The reason for this is that the body’s reaction to an injury is to try and protect the joint and the muscles around the joint contract to form a type of splint to hold the joint steady. Continued long term contraction of the muscles cuts off the blood supply and the products of muscle contraction build up in the area. These products cause pain and they cannot be removed as the blood supply is reduced. This is called muscle spasm. The muscle spasm in addition causes an increase force on the joint which sets up more joint inflammation and hence a vicious cycle of joint inflammation and muscle spasms.
Restriction of opening may be caused by muscle spasm, a change in lubrication within the joint due to inflammatory changes or the physical position of the disc blocking further opening and not reducing with a click.
The aims of treatment are addressed towards reducing joint inflammation and reducing muscle spasm.
Simple Treatment
The best way of managing a sprain of the joint is to rest it. It is obviously difficult to rest your jaw, as you have to talk and eat. There are, however, some simple measures, which will help to rest the joint as much as possible.
Softer diet
Try to take a softer diet, avoid steaks and instead have minced meat, try fish and mashed potatoes. You should avoid sticky toffees and chewing gum as these increase the amount of chewing. Crusty bread is often difficult.
Avoid Wide Mouth Opening
Try to avoid opening your mouth wide. Cut apples up into small pieces, avoid Big Mac’s etc and if you are about to yawn try to stifle this. Dental treatment should be divided into several short visits rather than one long one.
Clenching
If you notice yourself clenching your teeth during the day then stop, swallow and let the teeth rest apart in this position for 5 seconds. This rests the jaw by placing it in the most relaxed position.
Topical non-steroidal anti-inflammatories (NSAID)
Topically applied gels containing NSAIDs work very well to reduce the inflammation and pain in and around the joint. These have less systemic effects than taking tablets, such as Ibuprofen, and work just as well.
The gel should be applied over the area of the joint (in front of the ear) regularly four times a day and should continue for four weeks. Examples include ibuprofen, diclofenac and piroxicam gels.
The above two measures alone are usually helpful to reduce or even abolish pain in the majority of patients.
The above two measures alone are usually helpful to reduce or even abolish pain in the majority of patients.
We often use a lower soft bite-raising appliance (splint), which you should wear at nights only. This is a clear splint (like a gum shield), which is soft and fits over your bottom teeth. You need an impression, which can be taken by your dentist. A model is made of your lower teeth and the splint is made over these. You will be charged for this appliance by your dentist.
Initially some people find it difficult to keep this in their mouth and they find that they have discarded it by the morning. It is important to persist with the splint and it can take up to six weeks to start having some effect.
The splint works in three ways
1. Because it is soft it spreads the load and reduces the force that is being transmitted to the joint.
2. Because it increases the gap between the teeth it allows the muscles to stretch and therefore helps to reduce muscle spasm and it also helps to reduce clenching of teeth overnight.
3. By a mechanism of the lever and fulcrum principal the force exerted by biting the teeth together is now acting further towards the back of the mouth and therefore the load, which is passing through the joint, is reduced.
Conclusion
All these factors will be discussed in your clinic appointment.
A painless click of the jaw is not a concern however any jaw joint problem, which is related to pain, locking or restriction of opening may require operative intervention. Please see later article on causes of TMJ problems ( ‘Current thinking in the examination and treatment of TMJ Disorders’ ) there is a lot that can be done non surgically to rectify the problem as the majority of problems are ‘non-functional’ ie without an anatomical problem of the jaw joint.
Exercises to improve the function of the Temporomandibular joint
Set aside two 5 minute periods every day, at a time when you are relaxed and have nothing on your mind. One good time is just before you go to bed, another is perhaps when you get home from work. Sit upright in a chair and carry out the following manoeuvres:
1. Close your mouth on your back teeth, resting the tip of your tongue on your palate, just behind the upper front teeth.
2. Run the tip of your tongue backwards on to the soft palate as far back as it will go, keeping the teeth in contact.
3. Force the tongue back to maintain contact with your soft palate and slowly open your mouth until you feel your tongue just being pulled away from the soft palate. Do not try to open your mouth further. Keep it in this position for five seconds and then close your mouth. Relax for five seconds.
4. Repeat this manoeuvre slowly over the next five minutes in a firm, but relaxed, fashion.
As you open your mouth you should feel tension in the muscles at the back of your jaw and beneath the chin. For the first few times that you do the exercise you should check in front of a mirror that the lower teeth move vertically downwards—i.e. that there is no slight movement from side to side as you open your mouth. If the exercise is being carried out correctly, there will be no clicks or noises from the joints. If there is, you must be making some error in carrying out the exercise.
Do this exercise no more that the recommended amount for the first week. Initially, it may seem to make your pain worse, but this will be as a result of unaccustomed exercise. Thereafter, do the exercise as often as you can and this will help to strengthen the ligaments around your joints.
If the exercise is carried out correctly and regularly, over a two or three week period, you will retrain you muscles so that your jaw opens and closes smoothly without clicks or jerks and any pain that you are experiencing will subside.
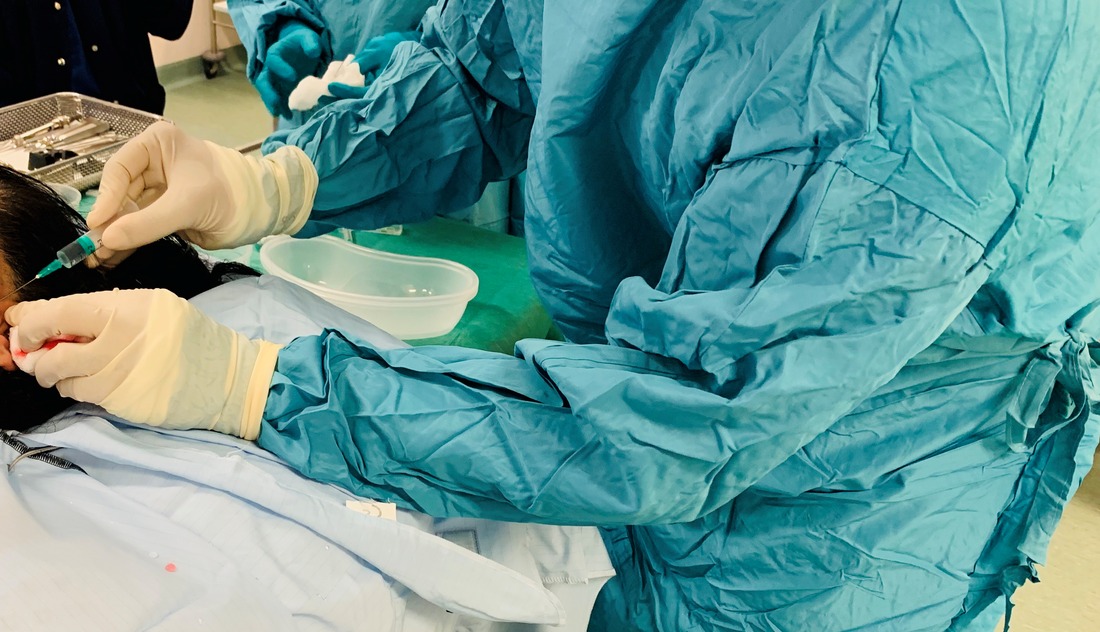
NON-SURGICAL TREATMENTS - BOTOX FOR MASSETERIC HYPERTROPHY SECONDARY TO GRINDING/CLENCHING
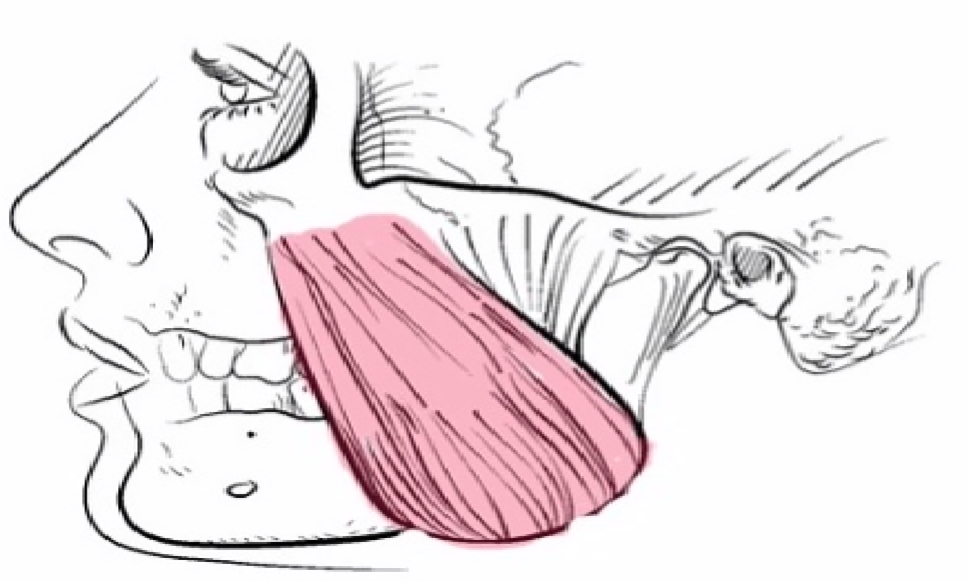
Botulinum Toxin for Massetertic Muscle Hypertrophy
This appearance is usually caused by large masseter muscles – one of the muscles involved in chewing. This muscle can become enlarged due to a chewy, fibrous diet or due to parafunctional activity including clenching or grinding your teeth at night. If you are aware, or have been advised that you clench or grind your teeth, this can result in headaches and pain in your face and jaw. It can also lead to damage to your teeth due to the high forces exerted on your teeth when clenching or grinding.
Botulinum toxin is used to relax the masseter muscle, and over a period of time, reduce its size. This will give the appearance of a slimmer face, as well as helping with symptoms you may be experiencing fromm grinding your teeth.
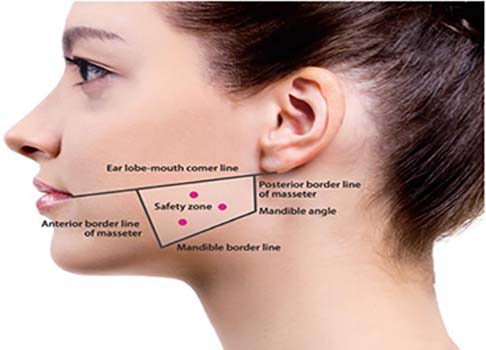
It is administered to the muscle in a very safe away over the danger zones of the face to reduce the chance of it diffusing towards the nerve of the face and causing temporary muscle paralysis.
It is similar to the technique used in anti-wrinkle injections, Mr Kassam will use a very fine needle and treatment is quick ( normally 5 mins ) with minimal discomfort.
You may experience some difficulty in chewing after the treatment but this is temporary. The force that you can chew will also be reduced as the muscle will be contracting less post treatment hence the muscle will become slimmer as a nice side effect normally of the treatment. This is normally referred to jaw line slimming treatment as well.
Surgical Treatments
TMJ Arthrocentesis
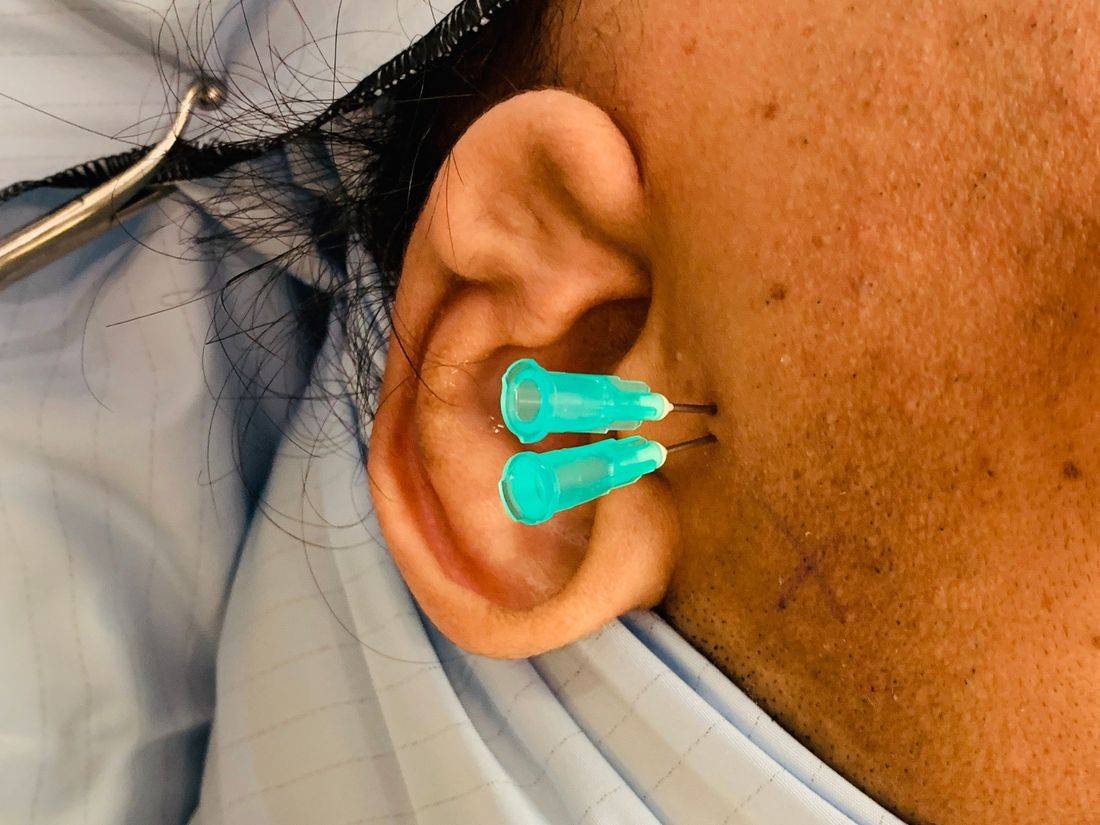
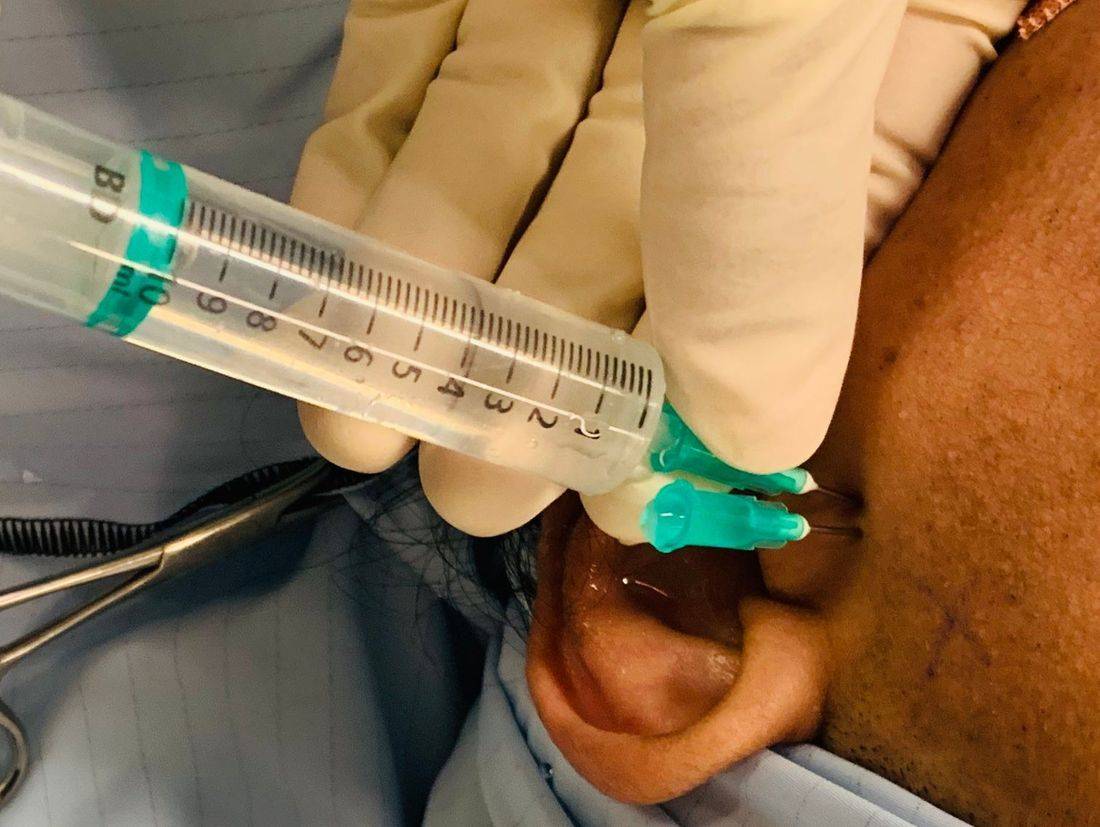
ARTHROCENTESIS (WASH OUT) OF JAW JOINT
This leaflet has been designed to improve your understanding of any forthcoming treatment and contains answers to many of the commonly asked questions. If you have any other questions that the leaflet does not answer or would like further explanation please ask.
The problem
The disc of cartilage which lies in your jaw joint has moved out of its normal position between the bones.
What is a jaw joint arthrocentesis?
An arthrocentesis is a procedure during which the jaw joint is washed out with sterile fluid. It aims to return the disc of cartilage to its normal position within the joint.
What does the treatment involve?
An arthrocentesis usually takes place under a general anaesthetic, ie you will be put to sleep completely. While you are asleep two small needles will be inserted into the jaw joint.
One of these needles allows sterile fluid to be pumped into the joint under pressure. The second needle allows fluid to be drained out of the joint.
Will anything else be done at the same time?
While you are asleep your lower jaw will often be manipulated in an attempt to encourage the disc of cartilage back into its normal position.
How will I feel after the operation?
The area in and around the jaw joint is often uncomfortable for a day or two after the procedure. You may find it necessary to take simple painkillers (eg Ibuprofen) during this time. There will also be some swelling in front of your car. You may also find it difficult to open your jaw for a few weeks.
Will I need another appointment?
You will need to return a few weeks after surgery to have your jaw joint checked by your surgeon. Arthrocentesis is not always successful and even in those people who have an improvement following the procedure it can take several months for this to occur.
TEMPOROMANDIBULAR JOINT ARTHROSCOPY
Level I arthroscopy
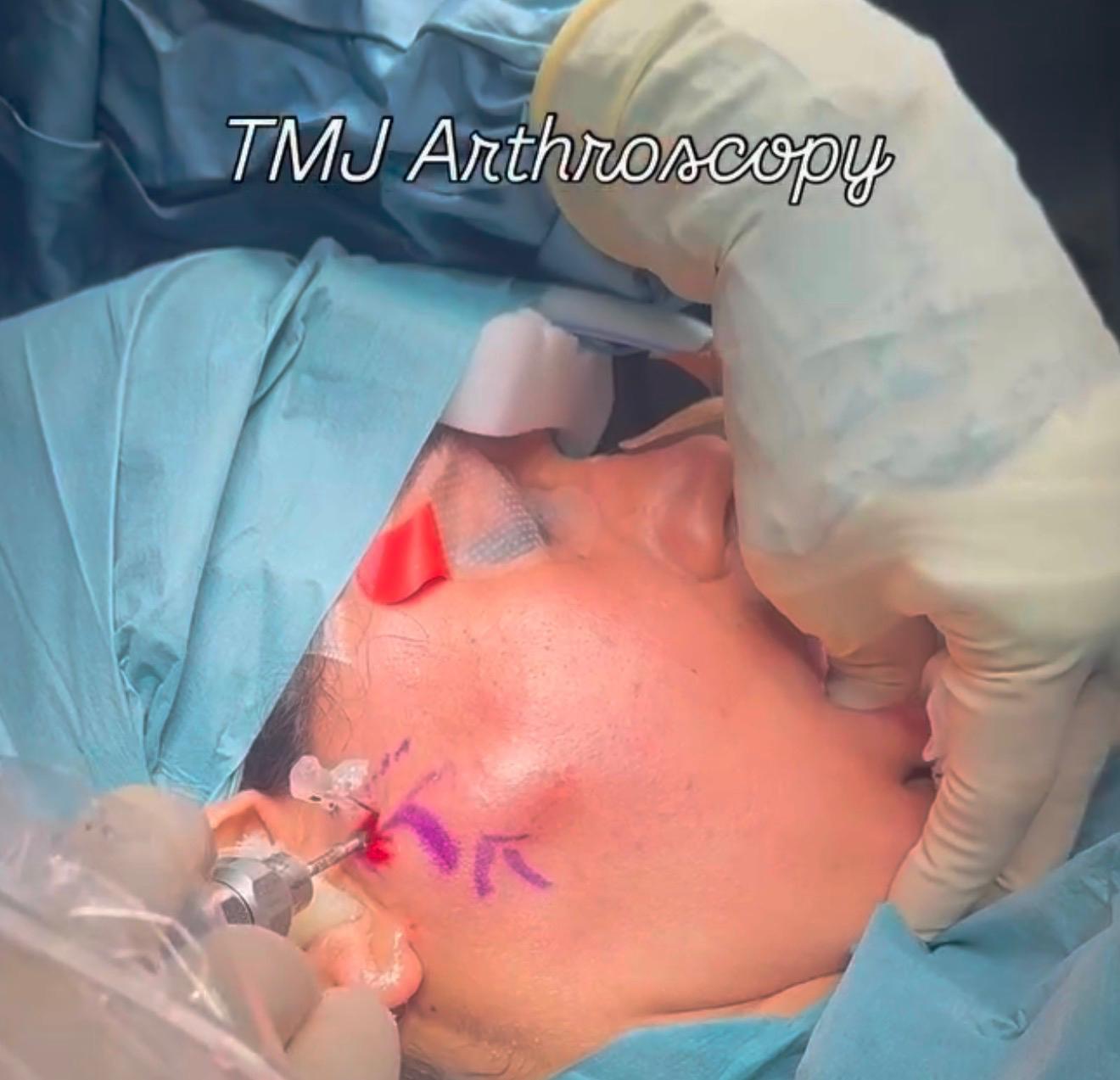
This is a basic diagnostic and therapeutic procedure. It can be used to assess the degree of cartilage damage, inflammation and even disc perforation to accurately plan future management and treatment. We can irrigate the joint under pressure and even use injections to the joint. You will need to carry out some jaw movement exercises after the procedure.
Level II arthroscopy
This involves an additional small incision, using a technique called triangulation. The procedure takes a little longer, but it allows for the use of coblation to remove problematic or unhealthy tissues without damage to the surrounding area. A biopsy is also possible with this technique and medication can be delivered directly into the joint. The recovery time can be a little longer and it may be slightly more painful afterwards.
What does the procedure involve ?

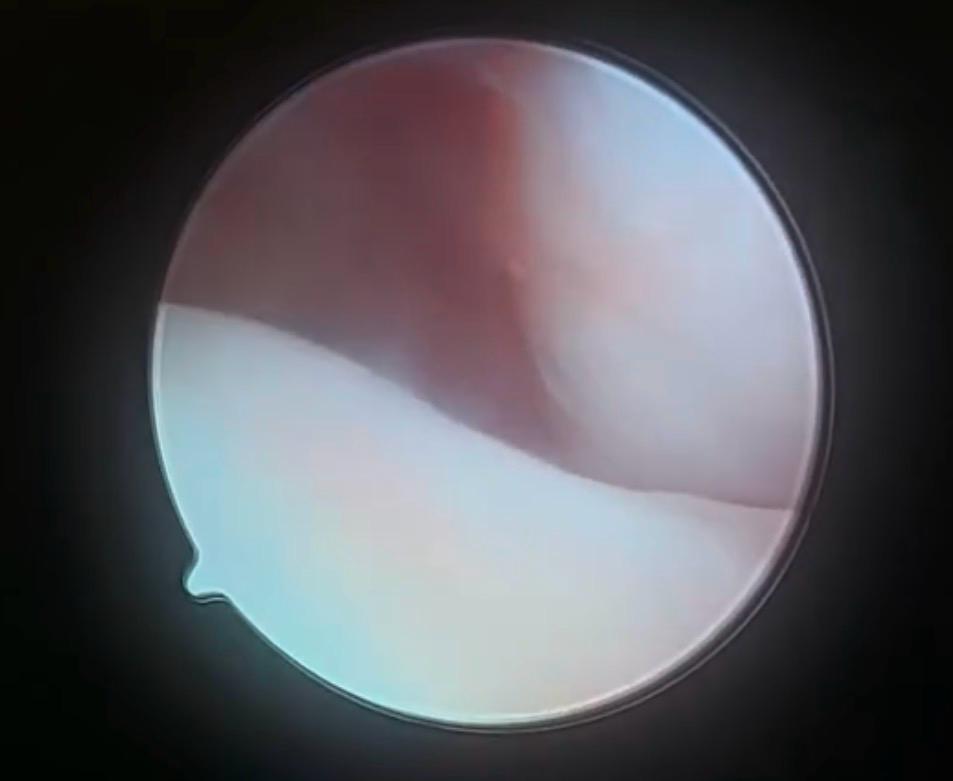
During treatment, we insert the tiny 1.9mm arthroscope into your jaw joint while you are under general anaesthetic and your muscles are completely relaxed. A small cut is made in front of your ear for this, enabling us to use the camera to look for damage to your jaw joint.
Arthroscopy is combined with arthrocentesis but this is no longer a ‘blind procedure’ and the joint wash breaks down any loose material or inflammatory particles that may be damaging the joint.
Jaw arthroscopy is considered a minor surgical procedure and you can go home to recover on the same day.
Frequently Asked Questions
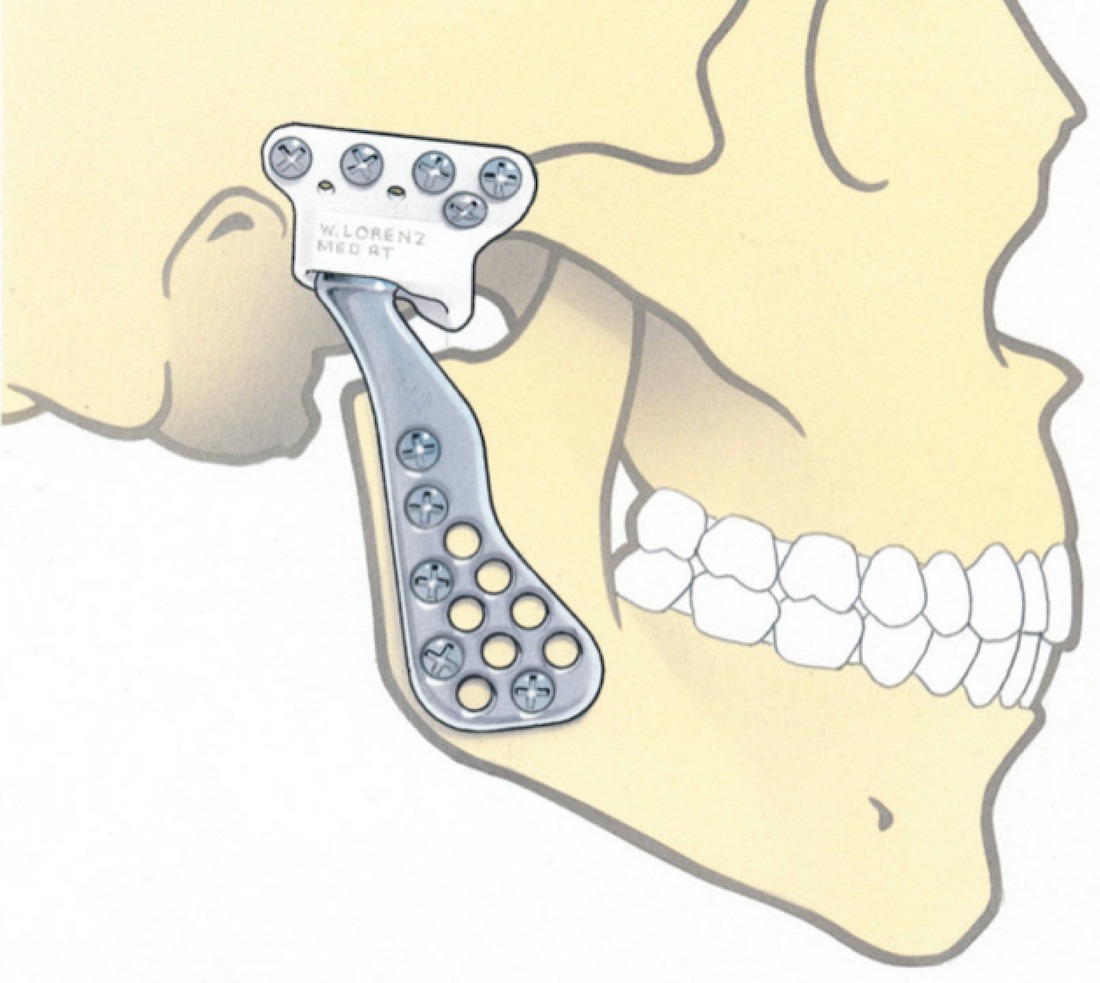
PROCEDURES - OPEN JOINT SURGERY & TMJ REPLACEMENT
Learn More Learn More
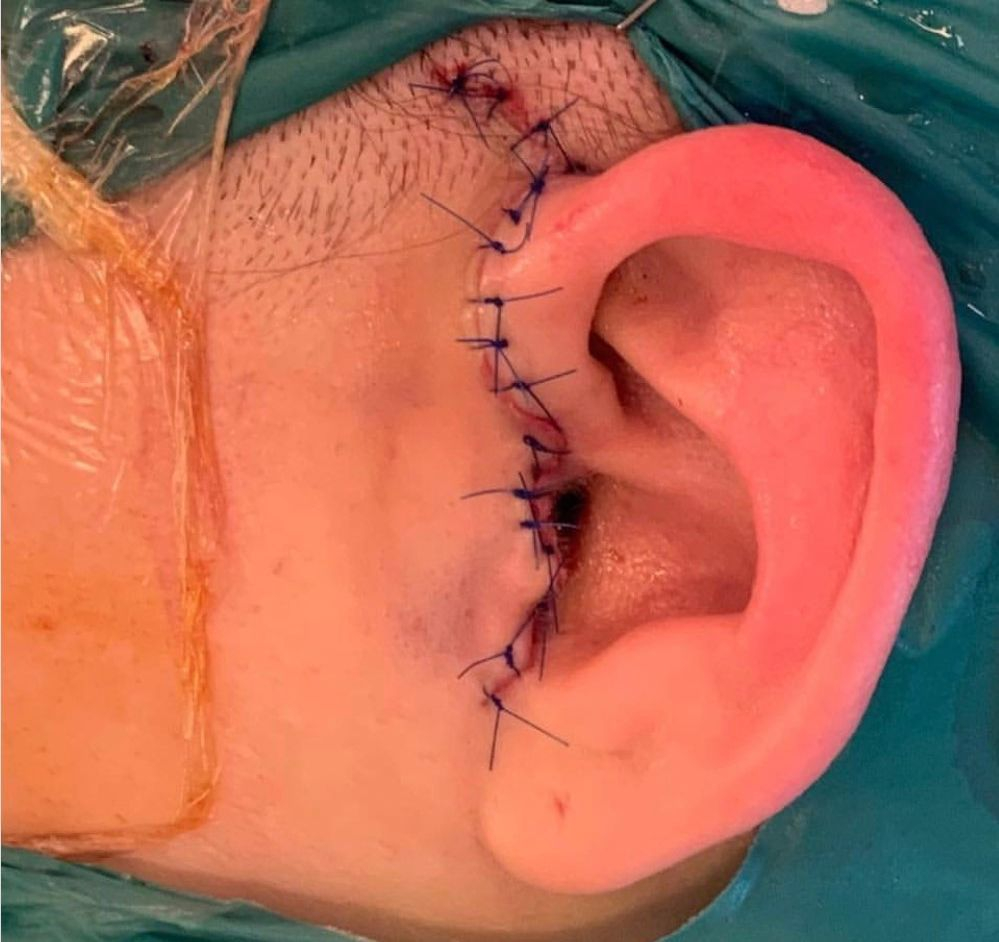
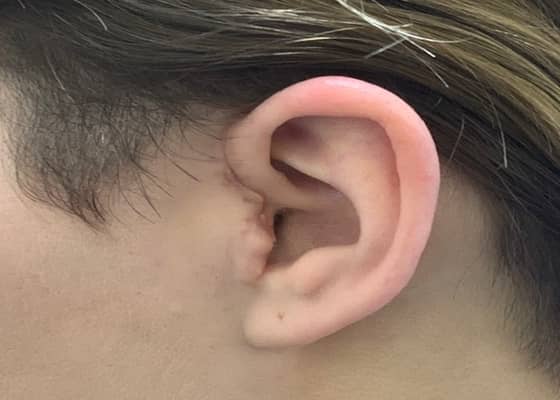
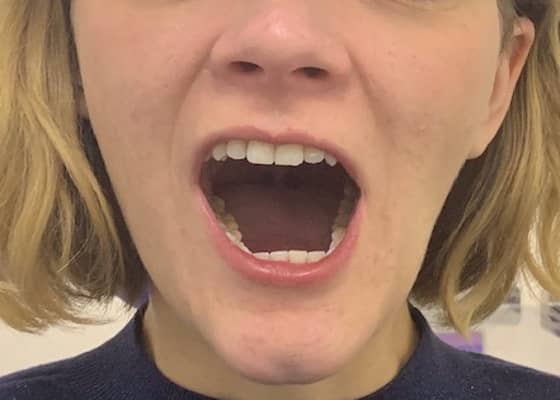
OPEN JOINT SURGERY 4 WEEKS POST PROCEDURE
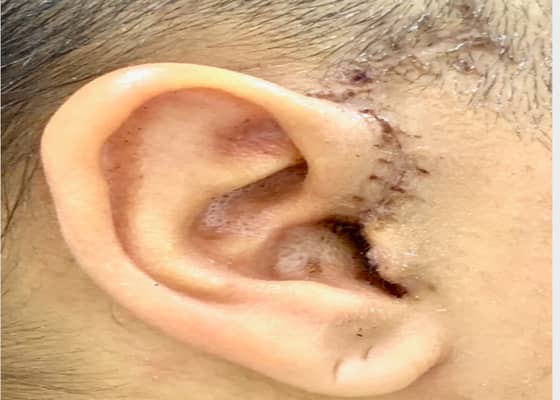
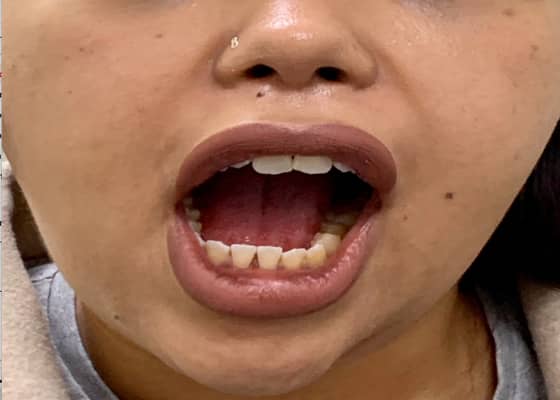
Learn More
Phone
07866807608 or 07956229992
The Harley Street Clinic
35 Weymouth Street
London
W1G 8BJ
London W1G 9QJ,
Clinics Hours :
Alternate Wednesdays 9am-1pm
Remote clinics : Monday - Thursday 6PM - 8pm
Click here :
To book into the Harley Street Clinic
The Harley Street Specialist Hospital
18-22 Queen Anne Street London W1G 8HU
Clinics Hours :
Alternate Thursdays 1-6pm
Remote clinics :
monday - wednesday 6PM - 8PM
Click here :- To book into Harley Street Specialist Hospital
London Independent Hospital
1 beaumont square, Stepney, London, E1 4NL
Clinics Hours :
Alternate Fridays 9am - 2pm
Remote clinics : Monday - Wednesday 6PM - 8pm
Click here :
To book into London Independent Hospital
The James Cook University Hospital
Marton Rd, Middlesbrough TS4 3BW, United Kingdom
Clinics Hours :
Alternate Monday To Fridays 6pm - 8pm

